Level 1, 10 Marine Parade, Southport, QLD, 4215, Australia
Tel: (07) 5531-0355

Arteries

Arterial Disease
Peripheral Arterial Disease
Thickening of the Arteries is an indicator of Vascular Disease and Heart Attack and Stroke. Peripheral arterial disease (PAD) (note peripheral vascular disease is called PVD), is a very common condition affecting 12-20 percent of Australians age 65 and older.
Schedule online. It's easy, fast and secure.
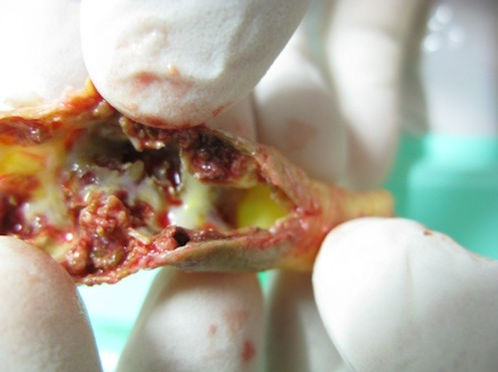
PAD develops most commonly as a result of atherosclerosis, or “hardening of the arteries,” which occurs when cholesterol and scar tissue build up, forming a substance called plaque inside the arteries that narrows and clogs the arteries. In the elderly we are now more commonly seeing calcified material that is similar to bone or a coral reef. Circumscribing large areas of the main aorta and its branches and in many areas developing as large masses and clumps that occlude the lumen of the vessel.
This is a serious condition. The clogged arteries can cause decreased blood flow to the all areas of the body; heart, brain,lungs kidneys and gut. In the legs, it can result in pain when walking, and eventually gangrene and amputation. Because atherosclerosis is a systemic disease, people with PAD are likely to have blocked arteries in other areas of the body. Thus, people with PAD are at increased risk for heart disease, aortic aneurysms and stroke. PAD is also a marker for diabetes,hypertension and other conditions.
Clogging of the Carotid Arteries can cause Stroke. When there are symptoms or very severe stenosis the Surgeon can offer treatment with Endarterectomy, Carotid Bypass or Carotid Stenting. Medical Treatment is used for lesser forms of the disease.
Examples of the atheroma or plaque that can cause stroke.

Symptoms
The most common symptom of PAD is called claudication, which is leg pain that occurs when walking or exercising and disappears when the person stops the activity.The most common other cause for similar symptoms is due to pressure on the spinal nerves from aging and degeneration of the back.
Other symptoms of PAD include: numbness and tingling in the lower legs and feet, coldness in the lower legs and feet, and ulcers or sores on the legs or feet that don’t heal.
Many people simply live with their pain, assuming it is a normal part of aging, rather than reporting it to their doctor.
Diagnosis
Diagnosis can be achieved even when there are no symptoms with the use of a simple screening test using continuous wave ultrasound. This is known as the ankle brachial index (ABI) test. This, painless non invasive test compares the blood pressure in the legs to the blood pressure in the arms to determine how well the blood is flowing and whether further tests are needed.
This dense white stuff is calcified plaque just like bone
Prevalence
• PAD is a disease of the arteries that affects 1 million Australians.
• PAD can happen to anyone, regardless of age, but it is most common in men and women over age 50.
• PAD affects 12-20 percent of Australians age 65 and older.
Risk Factors
Testing is appropriate in higher risk individuals and we can provide that in our ultrasound lab.
Your risk of PAD is increased if you are:
• over age 50
• Have a family history of vascular disease, such as PAD, aneurysm, heart attack or stroke
• Have high cholesterol or high lipid blood test
• Have diabetes
• Have ever smoked or smoke now
• Have an inactive lifestyle
• Have a personal history of high blood pressure, heart disease, or other vascular disease
• Have trouble walking that involves cramping or tiredness in the muscle with walking or exercising, which is relieved by resting
• Have pain in the legs or feet that awakens you at night
Treatments
• Lifestyle
Often PAD can be treated with lifestyle changes. Smoking cessation and a structured exercise program are often all that is needed to alleviate symptoms and prevent further progression of the disease.
• Angioplasty and stenting
Initial procedures were performed in the heart in Europe in 1974 and the equipment was progressively redesigned to cope with the more extensive disease and complex situations in the peripheral arteries. The competition between leading companies that supply the engineering and tools to treat this problem has been fierce in the last 15 years and we have lots of amazing equipment that can be applied with small punctures into the arteries rather than extensive open surgery.
This patient presented with rest pain and critical ischaemia in 2001; blocks in Series were treated 2 high grade stenoses stented in 2001 in the SFA artery; angioplasties below the knee:
2007 2 extra stents in SFA but crural vessels remain good and these are still patent in 2013
I have been fortunate to be at the leading edge of these developments since 1980 and participated in the progress from fairly crude balloon devices that were only available in small quantities to todays huge options of large systems to treat aortic stenosis and occlusions in the veins to the very long 200mm plus fine balloons designed to cross through extensive stenoses and occlusions in vessels 2 to 3 mm in diameter below the knee going into the foot.
Using XRay imaging for guidance, we use a fine specially designed wire, to pass through the obstructions, passed into the artery with a puncture and a sheath usually 1.5 to 2mm diameter.
Through the sheath and over the wire that can be considered like a railway line we can pass balloons to open the blockages and stents to support the arterial wall where they are needed. Stent technology continues to progress and there have been dramatic improvements since the 1990s when all that was available were rigid stainless steel stents, large copies of the style being used in the heart.
These rigid stents have been gradually replaced by flexible compressible high radial force stents in keeping with the dynamic forces that have been measured to affect the femoral artery and popliteal especially. The discovery that has allowed this is the development of a special metal alloy of nickel and titanium “Nitinol”. Not all nitinol stents are equivalent and they differ significantly depending on their design characteristics.
The stent is a metal cylindrical device, tiny in the heart arteries and in the arteries below the knee but above the knee to the aorta they can vary between 5 and 32 mm. In some cases especially aneurysms and for stents in the renal arteries a fine polymer covering is used making the device a stent graft.
This management is a minimally invasive treatment that has allowed us to limit the application of open surgery and in most cases I would use this “EndoVascular” approach first.
Blocked Calf Vessels below Complex Popliteal Aneurysm
Double blind trials have shown an equivalent outcome to open surgery but the EndoVascular procedures were carried out with non optimal procedures and the results if carried out with what I have available for routine use now would dramatically change the results in favour of the EndoVascular with a much lower risk of associated morbidity and mortality.
Calf Vessels Recanalised to the foot with Modern angioplasty techniques
Patient returned after this for Pop Aneurysm Repair

Surgery gives better results in the groin region where we often find large masses of occlusive calcium and stents are prone to fracture and failure at this site. Often we can combine Surgical and EndoVascular procedures using Xray in the operating theatre, Special “Hybrid” theatres are being developed to facilitate this and some will have CT scans incorporated to allow assessment during spinal surgery particularly where this involves combined vascular reconstruction.
Particularly in Combined arrangements with Spinal and Vascular Surgeons we have developed procedures that can resolve both the spinal and the vascular components and give a solution that can reduce Multiple Major Surgeries (e.g. aortic aneursym and multiple anterior disk reconstructions) to a Single Operation